Everything You Need to Know About Nursing Time Management | NURSING.com
What are you struggling with in nursing school?
NURSING.com is the BEST place to learn nursing. With over 2,000+ clear, concise, and visual lessons, there is something for you!
Nursing school prepares you for a lot of theoretical situations. It gets you familiar with the basics, starting off very slow. You start with how to do everything, then you start taking care of one patient… trying to encompass all of the things you’ve been learning into each interaction. It’s quite overwhelming doing this for one patient, let alone an entire patient load.
The NCLEX and nursing school prepares you to identify which situations need to be addressed first, but what about 2nd, 3rd, 4th, and 5th?
And which patient do you address first whenever everyone is fine?
And what do you do when you have 2 phone calls on hold, a physician with one of your patients requesting your presence, 4 meds late, one patient vomiting, another requesting pain meds, and another needs to go to surgery STAT…
As experienced nurses, we’ll discuss nursing delegation, prioritization, how to communicate with physicians and the health care team, as well general nursing time management tips… you know for when…
… everything is time-sensitive, but no one is in acute distress… you have about 56 tasks to complete, but not sure which way would be fastest and most efficient..
You quickly think about tasks, get started… and somehow, you’re already behind. Everyone’s situation has changed, and the tasks now need to be prioritized differently… you’re suddenly late… late…
And every day that date looks different… one day it’s a patient who needs to go to the OR, the next it’s someone who needs to be discharged STAT so you can make room for another patient, the next day it’s someone who has lost IV access and needs IV meds immediately…
We, as experienced nurses, are going to talk about some of these very important aspects of time management. Delegation, communication and prioritization are all important aspects, which nursing school discusses in a theoretical sense… but what is desperately needed, is for those of us with experience to explain it in a practical sense.
Because each state and facility have varying rules and regulations on what you can delegate, we are not going to elaborate on delegation, but it is still super important to consider when managing your time effectively.
Similarly, we won’t cover those obvious, drop everything and attend to this specific patient situations. The NCLEX and nursing school prepares you for that. Where our knowledge gap occurs are in those normal, every shift, kind of situations… those, ‘everyone is technically fine but there are 900 tasks to compete and I’m so overwhelmed I don’t even know where to start’ situations.
You start to feel like Alice, aimlessly wandering through Wonderland… not exactly sure what your goal is… trying not to get in trouble for forgetting something you had no idea you needed to do, and somehow you’re already late and slowly realizing…
Work Smarter, Not Harder
"One of the biggest keys to time management is working SMARTER not harder."
Click to Tweet
Efficiency, people! It is how you will survive and not clock out 2 hours late every shift.
In a lot of aspects of life, people like to tackle one task at a time… and once that tasks is completed, then look to the next one. However, this will NOT work in nursing.
I repeat – you cannot work with your head down, completing one task at a time… only looking ahead when you’re done with something.
You must have a strategic plan when looking at everything you have to do.
Consider…
Which tasks can be consolidated
- Can I change the patient’s dressings while giving a bed bath?
- Can take them to the bathroom after I give them meds?
- Can I check their blood sugar, complete an assessment, and give meds in one trip?
- They have 7:30, 8:00 and 9:00 meds… can I give them all at 8:00?
Bottom line: the less trips into the room, the faster you get things done. CONSOLIDATE.
What can I delegate?
- Is my coworker caught up? Can he or she give this IV Zofran for my puking patient while I deal with my other patient who is screaming at the top of her lungs?
- Can my CNA take the patient to the bathroom, switch out the sheets, and grab a blood sugar while I collect my meds and stuff to start a new IV on them?
- Occupational therapy is here, can they help the patient eat while they do their assessment?
Bottom line: leverage the other members of the team to get things done. Nursing is a team sport. You are not alone caring for your patients. You will help others, and they will help you.
Which tasks are the most important to complete? (Prioritization)
*I am not going to go over prioritization related to someone who is having ABC issues (airway, breathing, circulation) because those are drop everything scenarios… you are most likely a bit more well-versed on those, rather than when everyone is fine. For all intents and purposes, if someone is having an ABC issue, they are now the priority.*
- Are there any time-sensitive meds? (Insulin is a big one!)
- Do I have a bad feeling about anyone?
- Should I go see the patient that didn’t look so hot, but nothing specific was wrong during bedside report?
- Is anyone waiting on me to do something?
- Is the patient waiting on you to give a medication before they can go to dialysis?
- Is the CNA waiting for you to disconnect their IV fluids so the patient can shower?
- Is the patient waiting for you to give them insulin so they can finish their meal?
- Is the pharmacy waiting for me to chart an accurate weight so they can dose a medication?
- Is any single patient going to take substantially longer than the others?
- If one patient will require much longer to give meds (maybe they need it given crushed down a feeding tube rather than can just swallow independently), has multiple dressing changes, many IV meds, also needs to be changed/full linen change and bath, and so on… but your other patients are just some oral meds and an assessment, save the most labor-intensive patient for last so if you do get caught in there for quite a long time, you’re only late on 1 patient’s meds, rather than 4.
Bottom line: complete the most important, time-sensitive, someone-else-is-waiting-on-me tasks, as well as the quick tasks first.
We will go into more specifics about some key principles as well as additional information that will help you flow through your shift much more smoothly and with more confidence and control.
But, I know what you may be thinking… “it’s not about speed, I want to be able to spend time with my patients!”
Sorry… but there simply is not enough time to complete tasks by the time they need to be completed to allow for inefficiencies. There just isn’t enough time. At all.
In nursing school, it sounds ideal to forgo time management and just spend time with your patients.
However, once you’ve stepped on to the nursing floor, get report on 6 patients and suddenly learn that you need to start an IV, hang fluids, answer the 3 calls on hold for you, take someone to the bathroom, call pharmacy for a missing antibiotic, help your coworker pronounce their patient deceased, send a request to the blood bank for a unit of blood, and assess 6 patients, give their meds, document on them, and round with the physicians… that ideal nurse sit down and slowly complete tasks just to be with all of your patients mentality goes from something you wanted to do, to unfortunately, something you know you’ll never be able to do.
To put yourself in the best position so that if a patient does truly need to you stop everything and just be with them, you must be efficient in getting your tasks completed. There are many things to do for one patient, let alone 2, 3, 4, 5, 6… 7, 8, or 9 patients.
Aimlessly completing tasks, but being inefficient in them creates more work for yourself and will leave your patients having constant needs that you’re always behind on. Without time management, you’ll be that nurse who stays a 1-2 hours after each shift so you can chart.
Keep in mind that just because someone is an experienced nurse does not mean they are good at time management. There are very experienced nurses that are terrible at this. They always clock out late and are constantly overwhelmed.. Don’t just assume that because someone is experienced at nursing means they are good at time management.
This is like the classmate who “studies” all night every night for a week before an exam… but just reads and rereads the textbook, half awake, hoping to somehow memorize it… who ends up getting a terrible grade.
Compare this to the student who sets aside 2 hour blocks of time who focuses intently on learning the information for 20 minute increments with 10 min breaks… who focuses on learning the material in various ways (reading, highlighting, explaining to someone else, watches a video).
Alright, now that we both have a similar definition and know the importance of working smarter, not harder… come with me down the rabbit hole of time management…
Time Management Works Everywhere
There are whole books written on time management and it isn’t something that you only need in nursing, it’s something that you need in every single aspect of your life.
For example, when preparing an unbirthday dinner, you need to multitask to make sure everything is the proper temperature and done at the same time. Because preparing dinner is no tea party!
Or perhaps you are writing a paper due next week? You need to gather your resources, do the research, make an outline, schedule your time, etc. otherwise you will be wasting your time trying to ponder riddles such as why is a raven like a writing desk… which can cause people to think you have become stark raving mad! But don’t worry, this happens to the best of nurses.
Utilizing your time wisely can save you from becoming mad as a hatter. And besides, let’s be real here, you just haven’t the time!
So when your patient needs to have another bag of normal saline hung, stop and prepare for any other potential thing that patient might need before going into their room. This sounds simple until you are in the room and have forgot something, as hindsight is usually 20/20.
Hindsight is what gives us answers to questions such as ‘Why is a raven like a writing desk?’ which of course, Lewis Caroll admits he didn’t have the slightest idea originally but then many years later, due to popular demand, writes the answer to be, “Because it can produce a few notes, though they are very flat; and it is never put with the wrong end in front!” He came to this by many people offering up many answers and this answer to be the best fitting as well as the most popular. Similar to nursing, you will have many people offer up ways to help you work smarter, not harder. It is up to you to pick which answer is best for you and makes the most sense.
Using time management will keep you from running down the hospital hallway shouting, “No time to say hello-Goodbye! I’m late, I’m late, I’m late!” Which is exactly why the NURSING.com team prepared a cheat sheet to hopefully help you get from wondering why you are late to knowing your clock is exactly two days slow!
The recipe to fix this though is, of course, going to take some trial and error as you learn to prepare for a bed bath by collecting the soap, wash clothes, basin, mustard…
MUSTARD! No, let’s not be silly!
Towels, now that’s different…
There will always be advice along the way, and some you should take and some might not work for you. However sometimes, the March Hare (AKA Seasoned Nurse) is right and there is only one way to stop a mad watch!
Delegation
Delegation is a vital aspect of time management. You simply cannot complete all of the tasks and care for your patients without the help from others.
You need your coworkers, and your coworkers need you.
Remember, nursing is a team sport.
king at the million and one tasks, think about how you can incorporate the team.
An important aspect of delegation is communication. If you’re working with another nurse closely (like break partners, pod-members, or something similar), proactively touch base with them at the beginning of the shift. See what larger things they have going on with their patients today (someone transferring, taking a patient off the unit, helping a physician with a procedure). This helps you anticipate and plan better.
Do the same with your CNA. See what their day looks like so that you can help them with their tasks… for example, tag-team a bath and get your assessment done while you’re in there. The CNA feels supported and you’re both getting things done… and most likely getting them done faster if you had done this independently.
As you’re going throughout your day, try to keep in mind ways you can help your team. If you’re walking your patient to the bathroom and know your CNA has been meaning to switch their sheets out, take care of it for them. If you see your coworkers patient’s IV fluids are about to run dry and you’re heading to the med room, grab and hang a new bag for them. Be conscious of others and help them out. If you’re doing this, they are more likely to do the same for you… and ultimately, all of the patients get better care.
Do not make the most common rookie mistake…
The most common rookie mistake that nurses make is, out of a desire of not wanting to bother others, just doing everything themselves.
For example, if I knew my patient needed a bath and had to go to the bathroom and needed their sheets changed, I would just try to do all of that because I was too nervous to ask the nursing assistant to do it.
This is extremely inefficient. There are many things that you as the nurse must do, that the CNA simply just cannot. You have to find the balance of helping each other out, and trying to do everything yourself.
Similar to that mentality our patients have when they don’t want to put on the call light to bother us with something.
They think, “I don’t want to bother the nurses so I’ll just try to take care of this,” when it would be easier just to let us know what they need and then we can just take care of it much faster, and probably safer.
It’s the same thing with delegation.
Let your CNA’s and your support staff know what you need done so that they can take care of it much quicker than you would be able to when you also have many other tasks you have to complete that they cannot.
For example, When I was in my new graduate residency program, I was trying to take my patient to the bathroom and give him a bath when I was really far behind with my routine med pass. My amazing CNA came in the room and said, “Kati, what are you doing? You have so many things you have to do and I can take care of this! Go pass your meds!”
I was really thankful for that because she gave me this permission to delegate that I didn’t know that I already had. It just doesn’t make sense for me to do all of these tasks when there are others around that are part of the team that can do them.
You must delegate to survive. Your patient’s needs will not be met if you are attempting to provide total care, completely independently from everyone else.
Communication
As I mentioned before, communication is really important. Again, you will not be one nurse taking care of your patient load by yourself. You have to communicate with your team members continually throughout the day.
As you’re managing your time throughout the day and changing priorities as you go, make sure you’re communicating what you need to with your support staff. You CNA may not realize the sense of urgency in your tone of voice. Make sure you let them know when something needs to be done immediately. So if you need a quick set of vitals because you’re calling the physician, instead of saying.. “Hey can you grab a full set of vitals on Mr. Jones?” say something like, “I’ve got to call the doc about Mr. Jones. I think he’s septic. Can you get a full set of vitals for me right now? I want to page him STAT with those.”
It’s also good to make sure you’re on the same page as other people. What you think you’ve communicated or said
Nurse Physician Communication, on the Phone
In addition to communicating with the people you are elbow to elbow with, you must also communicate clearly with your physicians and their support staff. This communication can look different depending upon the unit you’re on. For example, if you are working in the emergency department, most of your physicians are at the nurse’s station with you and communication is frequently face-to-face.
However, if you work in a floor or in intensive care environment, your physicians and their support staff may not be with you. You most likely are going to have to page or call them. There are some important things to keep in mind, when you are paging these physicians and their support staff. We will go over communication on the phone as well as face-to-face, as there are some differences and ways to manage your time around that.

I’ve seen nurses make a very common mistake when it comes to communicating with physicians. Things come up throughout the day, which need to be addressed by the physician, some of these issues are urgent and some are not. However, some people think that whenever one of these issues comes up they need to call the physician right away for it to be addressed.
Right?
Wrong.
Let me give you a very practical example…
Your patient is scheduled to go to surgery this afternoon. They have a dose of subcutaneous heparin ordered at 1 PM. You’re not sure if the physician wants the patient to have this pre-operative dose. However, this physician typically rounds Around 11 AM. Some nurses may pick up the phone and call them right away, mid morning med pass. However, I argue that this is not the best way to go about this or manage your time.
This will require you to go page that physician, and wait for a response. Then you’ll have to hold the medication in the computer. If you’re made aware of this during your morning med pass, it will put you behind a bit to get it addressed… but the medication isn’t due for hours. There is also a chance you’ll see the physician a few hours before it’s due anyway.
However, if you simply wait for the physician to round, you’re not bothering him or her during whatever else they may be in the middle of. They will appreciate this consideration, as you’re not bothering them for something that could have waited. Also, you are not interrupted for a non-urgent need in the middle of the busiest time of the day.
Moral of the story: not every issue that requires a physician’s attention needs to be immediately addressed. Consolidate your non-urgent/non-time sensitive needs and requests to when the physician rounds.
Also, there are a few other things to keep in mind when paging physicians…
- Don’t page the physician and then go do something else that you can’t stop in the middle of (passing meds is a big example).
- Be prepared when they call back. It’s helpful to have the chart open or nearby, in case they are not at a computer themselves, but need to know things that aren’t off the top your head (like what their potassium was the last 3 days, or what their ins/outs have been running, or if the pharmacist changed the dosing to the vancomycin yet to reflect the latest trough). Also, make sure you’ve got a fresh set of vitals.
- If you’re not sure how to physically place a page, practice. I didn’t know how to do this until I actually had to do it. Most often, it’s inputting their pager number, waiting for beeps, and inputting your call back number. On where you work, you may need to chart when you paged them, as well as when they responded.
- Anticipate their questions – so if you’re calling about excessive urine output, be ready for them to ask you the input number, their total I&O’s for their admission, and the electrolytes
- Don’t just rattle off your question immediately – give them a second to remember this patient and their situation. They are seeing MANY patients and sometimes need a little background before they can answer your question. Tell them which patient you’re calling about, which room/unit they’re in, and ask if they’re familiar with them if you’re not sure. Give a brief sentence or two for background and ask your question (she had an AVR five days ago, flipped into afib last night and I’m calling you about the Amiodarone drip… or the patient was in an MVA three days ago, went to the OR for a femur repair, and now the wound looks red and has yellow drainage).
- Know when call starts. The MD’s will be off for the day after a certain time, then the on-call doctor is who you will call for any needs. If it’s getting close to the time the doctor’s will be off and the physician has not yet rounded, or you have some questions that are very routine… and you wait to call for clarification until after the doctor goes off for the night… that’s bad new bears. The on-call physician should not answer routine questions that could have been answered during the day. You must manage your time throughout the day, and ensure that your routine and non-urgent needs are addressed BEFORE the physician goes off for the day. Keep your eye on the clock!
Nurse Physician Communication, Face to Face
If you haven’t spoken to a physician before, it can be intimidating, to say the least. Especially if you are unsure of yourself. They can test you to find out what you know, your skill level and honestly sometimes just to be rude.
I know what it is like at the bedside battlefield. As a nurse, you get to hear the patient gripe and carry on while your hands are tied until the physician orders something. You’ve already paged the doctor and you’ve asked more than once. Still no order. You need to ask the physician in person. Now, if you have worked with the physician a ton, you probably have a working relationship, but if not, well, it can be stressful to say the least.
It is a completely different kind of battlefield when you try to talk to a physician in person. Even when paging the physician, you still have a lot of factors to consider, but when talking to them, face to face, a whole new level emerges, the nervous wreck level. Things you knew, you get messed up, things you didn’t know are, well… still unknown and make you look not so awesome.
Thus, when you finally approach the physician, nerves intact or not, and they ask, “Who are you?” You forget everything and give the most honest answer you have, quoting Alice, “Why I hardly know sir…I have changed so many times since this morning you see…”
After trying to explain to the physician how doth the little busy bee improve each shining hour, they inform you that they do not recite Against Idleness and Mischief by Isaac Watts, rather they have their own improved version that you have never heard before. Learning another way to recite a poem can be frustrating, and having different rules you play by per physician can drive anyone mad.
So what should you do if you are talking to a physician and you don’t know the answer? Start by admitting it. A good trusted saying I like to use is, “I don’t know the answer but I will find out for you.” Silence, lies, or any other form of cowering doesn’t help. Own up to it and let them know you will follow through.
The goal, however, is to avoid this, if possible. Try to get all the information before talking to the physician, try to have information ready to look up if needed.
Things to check before going to a physician:
- Past medical history
- Medications administered, amount and time of administration
- Home medication
- Your concerns/Patients concerns
- Lab results
- Vital signs (Both most current and trending)
This is a lot of things to check before you talk to a physician and the amount of time you have is limited, which is why it is vital for you to manage your time wisely.
Do not fret, it is near impossible to be prepared for every.single.thing, just possible to try to be prepared. Use our key principles list to get your time together so you can cover as many bases as possible.
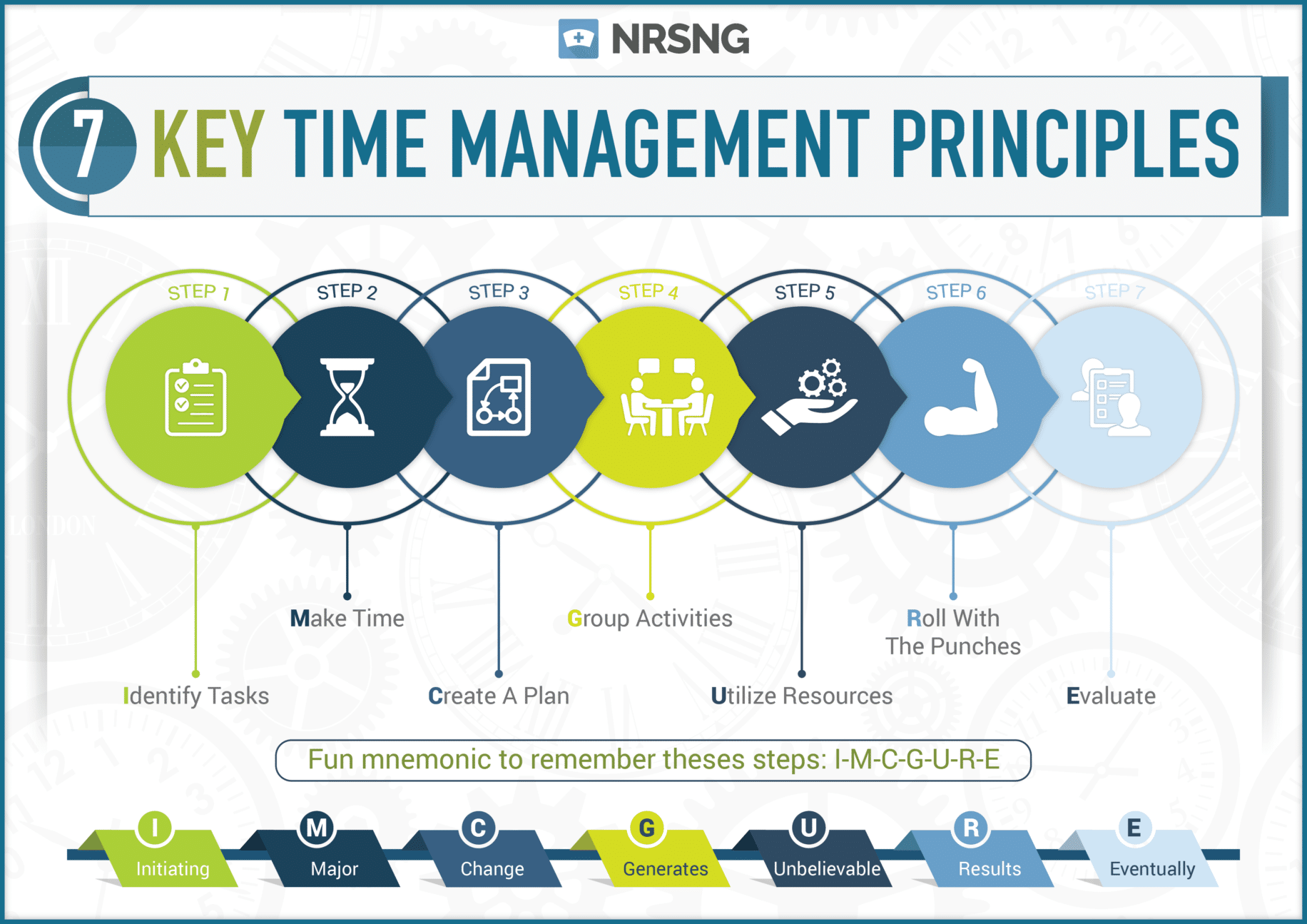
7 Key Time Management Principles For Nurses
It’s important, especially when you first start out, to have a systematic way to consistently approach your clinical experience to ensure you’re doing it appropriately. You’ve got to learn how to manage your time effectively, and it takes practice. We’ve developed 7 key principles in learning how to effectively manage your time and continuously improve. Let’s discuss…
Step 1 – Identify tasks
Figure out everything you need to do. This may change as you progress in your education. Your task list year 1 will look very different from second semester senior year.
Create a checklist on your report sheet so you wouldn’t forget anything. Eventually, you’ll be able to remember this all off of the top of your head – but not quite yet. I use a report sheet (here’s a link to a free database of downloadable brain sheets) and then hand write on the bottom my typical task list, then I photocopied it so I had it ready to go with each clinical and checked things off as they were completed.
Things I would include on this list were assessment, telemetry strip, education, routine meds, care plan, bed bath, and so forth.
As I realized I needed to complete non-routine things (timed blood draw, change an IV, insert a catheter), I would write these down as well and checked them off as they were completed.
Remember delegation when thinking about the tasks you must complete. Delegate appropriately and follow back up to ensure things were completed.
Step 2 – Make time
Think about how long each task will take. As you gain experience, things won’t take as long to do. But if you know you need to give meds to 4 patients, turn 2 patients, assess 4 patients, feed one patient, start fluids and give a unit of blood… think about how long it takes for you to complete those tasks and…
Step 3 – Create a plan
You’ve must come up with a plan of attack. After you’ve thought about how long each task will take, think about the order in which you will do them. Just as a nurse pro-tip, it generally works best if you save the most time-consuming patient for last.. If no one else has pressing needs. I typically peek into the room that I’ll save for last and let them know I will be in there in about an hour or two with all of their morning stuff and to hit their call light if they need anything before that. If they know you’ll be coming around, typically they’ll wait with non-urgent needs until you get there. That way, you’ll see and speak with all of your other patients, get their tasks done, and then can be in that one room longer without people feeling neglected.
Additional things to consider when creating this plan include…
- Time sensitive meds / procedures (insulin is due and a patient has their breakfast tray, or a patient lost IV access but is on a heparin drip)
- if you need others to complete a task (like a bed bath on a very large unresponsive patient, another nurse to sign off on your new PCA morphine cartridge)
- If you need to order anything (meds from pharmacy, supplies not routinely kept on the unit)
- If your patient is available (are they heading to dialysis in the next 20 minutes? Will they have an MRI and be off the floor for 1-2 hours?)
Step 4 – Group activities
Grouping things is an essential aspect of time management.
Consolidate tasks and trips.
If 3 patients need blood sugars and vitals done in the next hour, don’t go check all the blood sugars and then go check all the vitals. Check their blood sugar and vitals in the same trip. You’re interrupting the patient less, clustering care, and getting things done faster. It’s not about what you like to do in what order, it’s about what’s best for the patient.
Another example is clustering meds (disclaimer: facilities typically have policies in place about this.. So you have 30 min-1hr before and after a med is due to administer it before it’s either early or late. This is necessary because you physically cannot give 6 patients their 9:00 meds at once, you must have a window of time.) So, for example… you have 9:00 and 10:00 meds, give them both at 9:30 instead of two trips in the room. It sounds like it really shouldn’t take much time, but it adds up quickly… especially when you’re responsible for administering the 9:00 medications for 7 different patients.
Another example, common in the ED, is labs, meds, and procedures. So, if you know you’ll need to start oxygen, grab a set of labs, do an EKG, and administer 2 medications.. Grab ALL of the supplies needed to do those tasks and head into the room for 1 trip. This is exponentially faster. Additionally, you just will appear to the patient to have your stuff together, instead of leaving the room every 5 minutes to get more supplies.
Step 5 – Utilize resources
If you don’t know how to do something, look it up or ask someone where to find the information. Do not waste time aimlessly searching. Know how to quickly locate policies and procedures. If you are about to give a bed bath for the first time, ask a CNA what they routinely take in the room with them. If you’re about to start IV fluids on a patient for the first time, think about what you probably need and double check with a nurse. Or if you’ve come across a weird situation… like your patient that needs an MRI and has a house arrest ankle bracelet on, or your patient has maggots coming out of them and you don’t know what to do with them (yes, both of those things have happened to me) ask a more experienced nurse on the floor. Don’t just wing it and hope for the best.
Learn shortcuts for your computer charting system – being efficient with documentation pays off big time. If you notice someone has a trick, or “nurse hack” as I affectionately call it, use it! There is no pride in doing something in an unnecessarily inefficient manner.
Step 6 – Roll with the punches
Roll up your scrub sleeves and get to work! Start implementing the plan and be ready to pivot or change priorities at the drop of a hat. Don’t be so rigid with how you want to do things that you end up being inefficient simply because you weren’t able to finish your plan.
So if you were going to give your 1300 medication at 1330 and you see that the physician ordered STAT labs on that patient and it’s 1230, go give the med and draw the labs in the same trip.
Step 7 – Evaluate
Ok, so how did it go? Did you start implementing your plan and quickly realize it would have been better to see the patients in a different order? Did it take longer to do something than you anticipated? Did you learn a shortcut that you want to try out next time? Did it work better to take longer in one room, get additional documentation done at the bedside, than seeing all of your patients first and then attempting to document?
If you’re consistently reevaluating, you’ll find yourself incredibly efficient before you know it.
Do not miss this step! It is really important to stay on top of yourself and continually improve. Nurses that refuse to evolve and get better because they’re stuck in their way are the ones that clock out late, are always behind, and frustrated when change occurs.
Mnemonic
We also created a mnemonic to help you remember these steps:
I-M-C-G-U-R-E
I- Initiating
M- Major
C- Change
G- Generates
U- Unbelievable
R- Results
E- Eventually
Examples in the ED, ICU and on the Floor
I am sure you’re pretty well versed on going through examples of patient’s who are clearly the #1 priority… but let’s talk about some not-so-obvious scenarios. We will walk through the ED, the floor, then the ICU with some specific patient examples, and then talk about how we would manage our time in these scenarios. Let’s begin..
Location: Emergency Department
You take report on the following patients:
- 89 year old female who fell with coumadin on board. CT was negative for a brain bleed and X-ray showed a fractured pelvis on the right ischium. The patient received 4mg of Morphine, 4mg of Zofran and is admitted without a bed placement on the ortho floor yet. The patient just put on their call light and would like to order something to eat. Currently there is not a diet order in for this patient. Vital signs are the following:
- Temp: 98.6F
- HR: 88
- BP: 135/83 mmHg
- RR: 14
- Pain: 2/10 constant dull achy pain in the right hip.
- 81 year old female with altered mental status. Onset two days ago, negative for stroke symptoms and without a fall. The lab works showed +4 bacteria in the turbid dark yellow urine and a WBC count of 14,000 in the blood work. The patient is to receive 1g of Vancomycin after they finish the currently infusing 4.5g of Zosyn in 10 minutes. Patient is admitted to receive IV antibiotics on the urology floor and they have a bed that is ready. Report is called and transport is estimated to come in about 20 minutes. Vital signs are the following:
- Temp: 99.4F
- HR: 94
- BP: 110/58 mmHg
- RR: 18
- Pain: 0/10
- 40 year old male with a fever for 3 days. At arrival the temperature is 102.1F. The patient has received 1gm of Tylenol 1 hour ago and 1 L of normal saline. The last temperature recheck was 101.9F 30 minutes ago. Lung sounds are clear to auscultation, patient has a non-productive cough, and sinus pressure. The patient’s lab work resulted 5 minutes ago and the patient is negative for influenza and strep.
- Temp: 101.9F
- HR: 105
- BP: 120/80 mmHg
- RR: 20
- Pain: 3/10 generalized and achy.
After you have laid eyes on all 3 of your patients, introduced yourself, and updated them on the plan of care, you can implement our 7 key principles to help you get your assignments done effectively, smoothly, and with the least amount of wasted time as possible.
Step 1: Identify Tasks
You need to do the following:
- Patient 1: Hip fracture/fall
- Ask the physician for the diet status
- If able to eat: get an order
- Ask the physician for the diet status
- Patient 2: Altered mental status/UTI
- Get Vancomycin, a pump, and tubing
- Change before transport takes patient to the floor.
- Get Vancomycin, a pump, and tubing
- Patient 3: Fever
- Re-check a temperature
- If still high, ask physician for Motrin
- Re-check a temperature
Step 2: Make time
You need to prepare for everything and implement in 1 hour because you need to be able meet your hourly rounding per patient and since one patient will be leaving in approximately 20 minutes, you need to be prepared to get another patient.
Step 3, 4, & 5: Create a plan while grouping activities and utilizing resources.
The patient’s temperature needs to be re-checked prior to talking to the physician. You can delegate this task to a tech or medic. You also need to talk to the physician before getting the vancomycin because if they order motrin, you only want to go into the medication room to get the medications once. All of this needs to happen within 20 minutes because the Vancomycin needs to be hung before the patient goes to the floor. If patient can eat and an order is placed, ask either a patient representative/guest relations person or your tech/medic to get the patient a menu for ordering and/or getting them food from the nutrition room. Also delegate to an available person getting a pump for the vancomycin. The re-check temperature is 101F.
Step 6: Roll with the punches
Once you speak to the physician, they order the motrin but also another Liter of normal saline. The hip fracture patient is NPO for possible surgery. Slight change in plans, so you need to let the patient know they are unable to eat and you need to grab additional medications when you are gathering the other medications.
Step 7: Evaluate
It is tough to say whether you could have done some of those steps just as effectively while you were introducing yourself. This is a personal preference. I like to lay eyes on all my patients and tell them what I am going to do before I do anything so I can have a visual on them. However, there can be an argument made for stepping into the fever patients room and saying hi while taking a temperature then talking to the physician, then gathering medications, hanging the Vancomycin, then informing the patient they are NPO and lastly running medications into the fever patient. And to be honest, I’m sure there are plenty of other ways to order these tasks that make more sense to other people. This is why it is vital to figure out what works for you.
Location: Med-Surg Nursing Floor
You just clocked in and got a report on your four patients for the day. Here is a little bit about each patient and their current needs.
- 87 year old male with a stable ischemic right MCA stroke. Came in with left sided weakness and received tPA. His weakness has improved significantly since admission, but there is still some present. His speech is also impaired, but has been cleared to have mechanical soft foods and honey thick liquids, no straws. He most likely will transfer to a rehab facility later today. You’re working with case management and the family to ensure transport and and whatnot are set up.
- He has an 0730 PO Synthroid due
- His daughter is on hold, asking for an update
- He is in bed, but has requested to get up to the chair for breakfast
- 38 year old patient with a history of chronic alcoholism. He was intoxicated and fell, hitting his head on the curb. He has a resolving subdural hematoma, which was evacuated surgically 8 days ago. His frontal-temporal incision is healing well. He went into alcohol withdrawal 72 hours after admission but is no longer scoring on the alcohol withdrawal protocol and therefore doesn’t require PRN lorazepam anymore. His electrolytes are consistently abnormal and he flipped into uncontrolled atrial fibrillation with rapid ventricular response 2 days ago, was put on an Amiodarone drip and converted back to sinus. He is now on oral Amiodarone and will hopefully be discharged within the next day or so, but you’re a little worried about his home situation.
- He is complaining that his IV hurts (it is currently saline locked)
- His attending physician is at the nurse’s station, about to round
- 81 year old female who came in for altered mental status yesterday, diagnosed with a UTI. She was started on antibiotics. Her temp is 102.6F, HR 121, BP 102/72. She’s slightly confused, but that’s been baseline since she’s come in. She is resting comfortably. Family is asleep at the bedside, no acute concerns.
- You are concerned about her vitals
- 97 year old female patient with advanced dementia and stage IV cancer. She was admitted to your unit because hospice was full. She is actively dying. She is expected to pass at some point today. She is on hospice protocols, so she is only turned as needed and a blood pressure and heart rate check is only done once/shift and when/if the family requests it.
- She is grimacing
- She is diaphoretic
So you have received report and laid eyes on everyone! Let’s work through our steps…
Step 1: Identify tasks
-
- Patient 1
- Med due
- Phone call
- Out of bed to chair
- Patient 2
- Look at his IV
- Round with physician
- Patient 3
- Look at her vital sign trends, physician notes, labs
- Potentially call physician
- Patient 4
- Administer pain med
- Towel off perspiration, ask family if they would like us to bathe her
- Patient 1
Step 2: Make time
Patient 3 is the priority, due to her concerning vitals. However, patient 2’s physician is currently rounding and patient 4 needs pain meds soon.
Steps 3, 4, and 5: Make a plan, group activities, gather resources
Let the medical unit secretary inform them that that he had an uneventful night and to call back in 1 hour for a more detailed update. Delegate getting him out of bed. Grab the med that’s due when going to the med room for the pain med for patient 4.
Round with the MD for patient 2, look at his IV while in the room with the doc.
Grab the pain med for patient 4 and the Synthroid for 2 at the same time. Go to patient 4’s room to administer pain med. Towel off patient with a cool cloth and inquire about bath while administering med.
On the way back to the nurse’s station, do a full assessment of patient 3. Review her chart in the room. Page the physician once back to the nurse’s station. While you’re waiting for the return call, chart your assessment.
Step 6: Roll with the punches
Your CNA wasn’t available to help get patient 1 out of bed. You let him know you were going to check on your other patients and you’d be back shortly to help him. He’s slightly annoyed.
You continue with the plan. After the return call is received and physician is notified of concerning vitals on patient 3 (and a few orders have been received), you go administer Synthroid to patient 1 while you wait for patient 3’s orders to be verified by the pharmacist… the CNA is currently walking him to the chair, as she suddenly became available. This enables you to quickly administer the synthroid, complete a quick assessment and then go grab the newly verified meds for patient 3.
Step 7: Evaluate
How did it go? Well, it would have been better if before getting report you saw that patient 1 had a Synthroid due right away… you could have grabbed that before report so you could administer it to him at that time. Otherwise, things went rather quickly/smoothly.
You could have dropped everything the second you noticed something with patient 3 was off, however balancing those tasks with the time it took to get a full assessment and chart review completed so you could communicate appropriately to the MD, as well as leveraging the time you anticipated the order verification would take to attend to your other patients enabled you to continue providing care to everyone else simultaneously. Once patient 3 was situated, everyone else was caught up rather than quite far behind.
Location: Intensive Care Unit
You’ve just received report on your two patients. Below is a bit of information about each of them and what they need right at the beginning of the shift.
Patient 1
72 year old male patient that was found down and unresponsive yesterday. He was brought to the ED via ambulance and a CT scan revealed an extensive intraparenchymal hemorrhage. His blood pressure was 254/109 on admission. He was immediately intubated, as he was not protecting his airway. He currently on 15mg/hr of Nicardepene with an order to keep his SBP less than 150, intubated, and sedated with Propofol with a RASS of -2 (ordered to be at -2 as well), he has a central venous catheter in his subclavian. His current blood pressure is 142/86, HR 92, O2 100%. You have orders to insert a feeding tube, start tube feedings, administer 40 mEq oral Potassium and 25 mg lopressor down said tube, turn him, assess him. His wife is on the phone.
Patient 2
That same little 81 year old female that was admitted a few days ago with altered mental status and a UTI is now in septic shock in your ICU. She was urgently transferred to the ICU overnight after she was unresponsive to fluid boluses on the floor and had a decreased level of alertness. She was intubated upon arrival to the unit and a central line was placed. She is on 0.04 units/hr of vasopressin and 5 mg/hr Levophed with an order to keep her MAP above 65. She has an antibiotic due and a follow up lactic acid to be drawn and sent in the next 15 minutes. Her family is emotional and at the bedside. Her blood pressure is currently 95/44, HR 110, O2 96%, temp 101.8F (Tylenol suppository ordered for any temp over 99.2F).
Step 1: Identify tasks
Patient 1
- Place feeding tube, verify placement
- Administer meds
- Talk to wife
- Assess, turn
Patient 2
- Draw and send lab
- Hang antibiotic
- Titrate Levophed
- Administer Tylenol supp
Step 2: Make time
Let the medical unit secretary take a message from bed 1’s wife – you currently do not have time to be on the phone right now. Patient 1 is a little more tasky and stable, while patient 2 has some immediate priorities. Unless patient 1 has a spike in blood pressure, patient 2 is the priority.
Steps 3, 4, and 5: Make a plan, group activities, gather resources
Patient 2 is the priority. Increase Levophed to 6 mg/hr while you’re in the room. Go to the supply and med room, grab the Tylenol, lab stuff and antibiotic. Go back into the room, draw the lab, administer meds and simultaneously complete and assessment and turn. After this, check your blood pressure to make sure it’s come back up. (It’s now 102/58.)
Go drop the lab off at the tube station and grab the feeding tube for patient 1. Ask your CNA or a coworker to meet you in that room in few minutes. Place the feeding tube, assess the patient, and turn the patient on his side. When you’re done, peek at the blood pressure for patient 2. If it’s okay, then chart what you just did and order x-ray verification of placement of the tube.
Go back to patient 2, chart your assessment and check to see if the lactate level has come back. If enough time has passed to enable you to recheck a temp, do so.
Step 6: Roll with the punches
After you increase the Levophed for patient 2 and acquire the tube and meds for patient 1, you check the chart to verify the order to place the feeding tube on patient 1. You notice that in his history he had a sinus surgery 6 days ago.
You paged the physician (who changes the PO med orders to IV) and try to obtain medical records of this recent surgery to see if it is safe to insert the tube. You then assess, turn and chart on him. Next you check on patient 2 and complete those tasks. After you were done with patient 2, you go back to patient 1 to give the newly ordered IV meds.
Since you are caught up and they are both stable, you call patient 1’s wife back and provide an update.
Step 7: Evaluate
How did it go? It would have been helpful if you noticed the recent sinus surgery earlier on his chart (or better yet, if the MD that ordered the feeding tube did!). Since you were in the room, you went ahead and quickly assessed and turned him, but you probably could have just stayed with patient 2 until she was completely squared away once you realized you couldn’t place the tube.
Conclusion
You are either reading this because you are 1) afraid you will have issues with time management. 2) have issues with time management or 3) are floundering as a nurse or nursing student and really don’t know how to fix it. We are glad you are here. Seriously. We wrote this because we know it is a real problem for many nurses and have also experienced it ourselves! We got together to spill our secrets on time management to hopefully ease frustration and encourage excellence!
Do not be discouraged. Mistakes are going to happen, that is how people learn. If there wasn’t conflict, many amazing things would have never happened in the world. Such as the as seen on TV Clapper. What would our world be without this glorious device? I don’t even want to know…
You might be onto something amazing, so prepare as best you can and let your lessons and the lessons of others shape you into one efficient and kick arse nurse! Also, can someone please invent tangle free ECG machines? I have had this conflict with no resolution for far too long!


.png?width=50&height=50&name=stencil.amz%20(3).png)