BiPAP vs CPAP | An Overview of Non-Invasive Respiratory Support | NURSING.com
What are you struggling with in nursing school?
NURSING.com is the BEST place to learn nursing. With over 2,000+ clear, concise, and visual lessons, there is something for you!
Complete Confidence with CPAP vs BiPAP
An overview of non-invasive respiratory support for nursing students
Let’s be honest . . .
Ventilation can be a tough subject. I have said before, that the RT (respiratory therapist) should be your best friend on the clinical floor. Understanding the various modes of ventilation and which is best for a given patient or disease process can be confusing.
Click Above to Play the Episode
View NURSING.com Respiratory Course
This episode is designed to give you an overview of the differences between CPAP and BiPAP so that you will be able to walk into a room and feel comfortable with how your patient is ventilating.
CPAP vs BiPAP
First of all, let’s define what these terms stand for:
CPAP – Continuous Positive Airway Pressure
BiPAP – Bilevel Positive Airway Pressure
It’s also important to mention here that both CPAP and BiPAP are NONinvasive modes of ventilation . . . which just means that we are not required to insert a tube (endotracheal tube for mechanical ventilation). The patient simply requires a snug (very snug) fitting face mask or nasal pillow in order to be on this therapy.
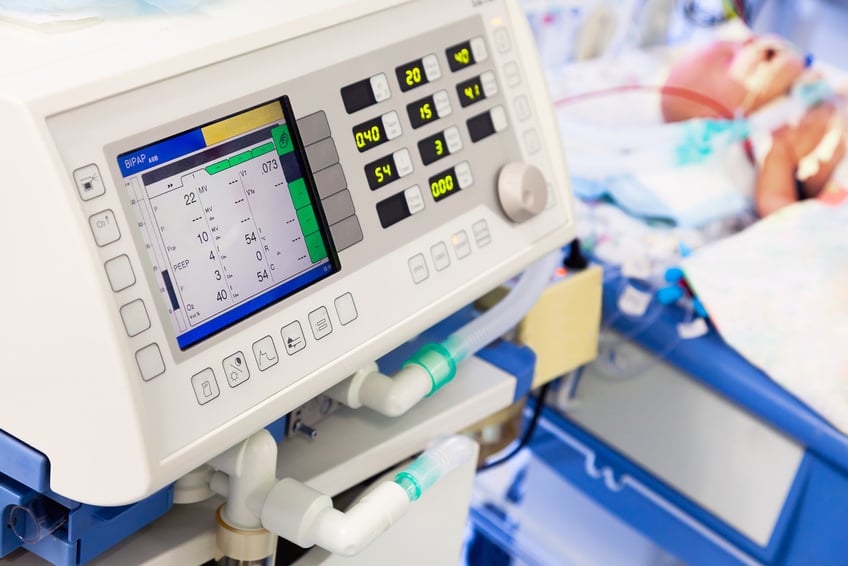
Continuous vs Bilevel
The major difference to keep in mind between these two is that CPAP is delivering a set pressure CONTINUOUSLY . . . it never changes. It doesn’t matter how fast the patient breaths, whether they are taking a breath, or if they stop breathing . . . it will just keep pumping along at the same pressure.
Bilevel on the other hand is much more sophisticated. BiPAP will deliver a DIFFERENT pressure depending on whether the patient is taking a breath or exhaling.
These two pressure differences are known as IPAP and EPAP.
IPAP – Inspiratory Positive Airway Pressure
EPAP – Expiratory Positive Airway Pressure
This is important for nurses and nursing students to understand because this is the KEY difference between these two therapies and is the foundation for their uses.
Uses for CPAP
Because CPAP only delivers one pressure setting it is important to understand that it helps best in situations of hypoxemia as it will aid with oxygenation.
CPAP will do the following:
- ↑O2
- ↓ Work of breathing
- ↑ Intrathoracic Pressure which will ↓ preload thereby ↓ cardiac workload
Due to these effects of CPAP, it can be useful in situations of sleep apnea and CHF exacerbation.
The only real setting for CPAP that the nurse needs to keep in mind is the initial pressure setting . . . measured in cmH2O.
Remember . . . CPAP is spontaneous . . . which means the patient does not receive any ventilatory support.
Uses for BiPAP
Due to the key difference between CPAP and BiPAP ( one pressure vs two pressures) , BiPAP is a great tool for ventilation (removal of CO2) in conditions like COPD exacerbation or other situations where the patient needs ventilation support.
Settings for BiPAP written by the physician will look like this:
Bipap 10/5 rate of 12 FiO2 of 60%
Notice the two pressures (IPAP vs EPAP). The difference between these two numbers is called PRESSURE SUPPORT.
In the order above PS is 5 . . . IPAP – EPAP or 10-5.
Notice also that the physician has ordered a RATE. This is a big difference between BiPAP and CPAP. With BiPAP, a specific rate is programmed in the machine and whether or not the patient is breathing, the machine will deliver the programmed pressure at the set rate.
Also, notice the order has a set FiO2 . . . this is the % of O2 to be delivered. Normal room air has a FiO2 of about 21%. The FiO2 will be titrated to keep the patient's SpO2 (pulse ox) or SaO2 (blood gas) at or above 91%.
If the patient continues to have difficulty maintaining appropriate SpO2 or SaO2 . . . the FiO2 can be adjusted.
If CO2 levels are high then IPAP and EPAP can be adjusted accordingly.
As Pressure Support increases (the difference between IPAP and EPAP) the lungs will be able to expand more to allow increased ventilation (clearing of CO2).
View NURSING.com Respiratory Course
SIMV vs AC
The goal of both SIMV and AC ventilator modes is to ensure proper ventilation/gas exchange for our patients. The major difference has to do with the tidal volume and how/when it is delivered. This concept is discussed in the episode along with some of the common vent settings like PEEP, Pressure Support, Tidal Volume, and FiO2.
Never Trust SpO2 and Oxygen Delivery DO2 Video (cardiac SaO2, SpO2, PaO2))
Conclusion
As I mentioned above . . . we have RTs and Practitioners for a reason. . . . this can become very complex very quickly. However, it is VITAL that you understand the basic settings and differences between CPAP and BiPAP.
You should know exactly what your patients' settings are and if/when adjustments have been made. It is also important to know WHY the patient was placed on ventilatory support as this will help you assess your patient and notify providers of any possible needed changes in settings.
As the nurse . . . are at the bedside . . . you are with the patient . . . it is your job to know what is going on with your patient. It isn’t required to have a complete, in-depth understanding of all of this . . .but as you begin to understand better what is going on you will be able to better take part in the patient's care.
If you haven’t signed up to receive our Friday Freebie emails . . . do so NOW . . .click here.



