Master pharmacology fast with visual drug cards, nursing implications, side effects, and memory tricks for 200+ medications.
The NCLEX often focuses on high-risk medications, commonly used drugs, and those with significant nursing implications. Here are the top medications every nursing student must know cold.

Avoid or limit vitamin K-rich foods (e.g., spinach, kale, broccoli) as they reduce effectiveness. Maintain a consistent diet.

Hold if heart rate <60 bpm or systolic BP <90 mmHg, unless otherwise directed by the provider.
No, stopping suddenly can cause rebound hypertension, angina, or even myocardial infarction. Always taper off under medical supervision.

Nephrotoxicity, ototoxicity, and infusion reactions like Red Man Syndrome. Promptly report hearing changes, such as tinnitus or vertigo.

Typically used every 4–6 hours as needed. Overuse can lead to paradoxical bronchospasm or reduced effectiveness.
Use a spacer for proper delivery, inhale deeply while pressing the inhaler, and hold breath for 10 seconds. Rinse mouth afterward to prevent irritation.

It reduces blood pressure and decreases the workload on the heart by preventing the conversion of angiotensin I to angiotensin II, a potent vasoconstrictor.

Contrast dye can impair kidney function, increasing the risk of lactic acidosis. Hold metformin for 24–48 hours before and after the procedure until kidney function is confirmed as normal.

Avoid in patients with glaucoma, tachycardia, or urinary retention, as it can worsen these conditions.

It’s commonly combined for synergistic effects, particularly in severe infections (e.g., endocarditis). This helps broaden coverage against resistant bacteria.

Headache, constipation, dizziness, and in rare cases, QT prolongation (monitor EKG in high-risk patients).
Yes, it’s often used to treat hyperemesis gravidarum (severe pregnancy-related nausea). Always confirm with the provider.

Treats anaphylaxis, cardiac arrest, and severe asthma attacks by increasing heart rate, improving blood flow, and relaxing airway muscles.
Administer intramuscularly (IM) into the thigh (0.3 mg for adults, 0.15 mg for children). Repeat every 5–15 minutes if symptoms persist.
Tachycardia, palpitations, anxiety, tremors, and increased blood pressure. Monitor for arrhythmias in high-risk patients
Pharmacology makes up 15-20% of the NCLEX. Get video lessons, mnemonics, and practice questions for every drug class.
Here are the Top 10 Medications Every Nurse Should Know. These medications are widely used, essential for patient care, and are likely to appear on exams like the NCLEX or in clinical practice. The NCLEX often includes high-priority medications such as beta blockers, ACE inhibitors, insulin types, and anticoagulants. Nursing students should be familiar with nursing implications, side effects, and common trade names. These free printable drug card PDFs will help you prep for NCLEX.

Heparin: The dose is typically weight-based (e.g., 80 units/kg bolus, then 18 units/kg/hr infusion). Always use the protocol provided by your facility and confirm with another nurse. Adjust the dose based on aPTT values to keep them within the therapeutic range (1.5–2.5 times normal).

If the patient takes more than 4g/day, has liver disease, drinks alcohol heavily, or uses multiple medications containing acetaminophen.
Yes, but check labels for hidden acetaminophen to avoid overdose. Many cold medicines already contain acetaminophen..

Hold if heart rate <60 bpm or systolic BP <90 mmHg, unless otherwise instructed by the provider.
No. Stopping suddenly can cause rebound hypertension, angina, or even a heart attack. Always taper off under medical supervision.

It strengthens the heart’s contractions and slows the heart rate, improving cardiac output and reducing symptoms.

Insulin mixtures combine rapid- or short-acting insulin with intermediate-acting insulin in one injection to simplify dosing and provide both mealtime and basal glucose control.
Administer 15–30 minutes before meals, depending on the rapid- or short-acting component’s onset time.
If mixing insulins manually (e.g., rapid/short-acting with NPH):
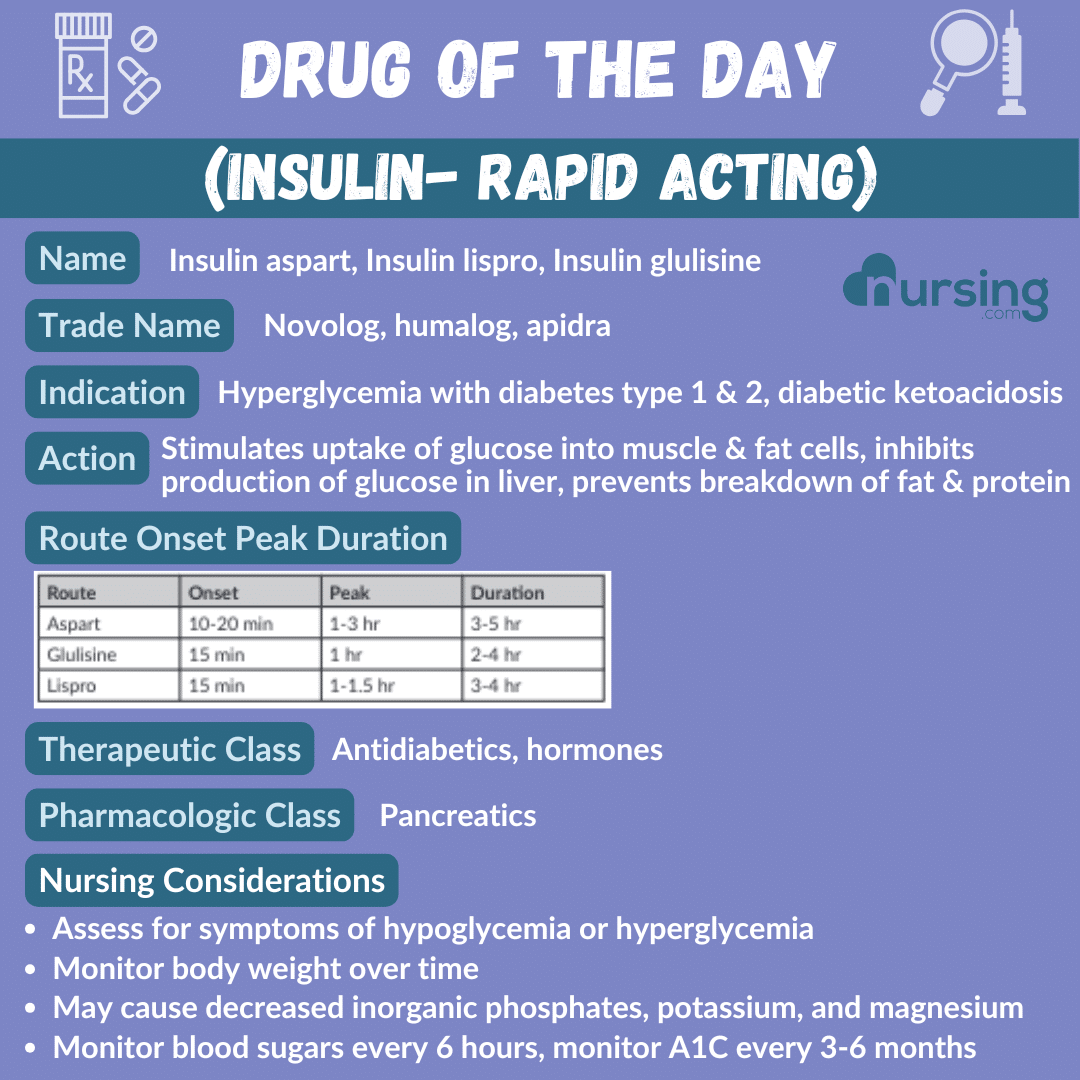
Administer immediately before meals to control blood glucose spikes from food intake.
Yes, it can be mixed with intermediate-acting insulin (e.g., NPH) in the same syringe, but administer immediately after mixing to maintain effectiveness.

Typically given once or twice daily, often in combination with rapid- or short-acting insulin to provide basal control between meals and overnight.

Typically given once daily (sometimes twice for some formulations). It provides basal glucose control throughout the day and night, mimicking the pancreas’ natural insulin release.
No, long-acting insulin (e.g., glargine or detemir) should not be mixed in the same syringe with other insulins as it can alter its effectiveness.

It helps track fluid balance and detect early signs of dehydration or fluid retention.
Encourage adequate fluid intake unless restricted, monitor for signs of dehydration (e.g., dizziness, dry mouth), and adjust dose as prescribed.

To reduce the risk of stomach irritation, ulcers, and GI bleeding.
Black, tarry stools, vomiting blood, abdominal pain, or unexplained fatigue.
Yes, but they should be taken at different times to avoid overlapping doses and always under a provider’s guidance.

Pharmacology makes up 15-20% of the NCLEX. Get video lessons, mnemonics, and practice questions for every drug class.
Understanding drug classes helps you predict side effects, nursing implications, and contraindications . . . even for drugs you've never seen before.
ACE inhibitors block the conversion of angiotensin I to angiotensin II, lowering blood pressure by reducing aldosterone levels. A side effect is a buildup of bradykinin, which can cause a cough or angioedema in some patients
ARBs block angiotensin II from binding to AT1 receptors, lowering blood pressure and aldosterone levels. They have fewer side effects than ACE inhibitors but can cause high potassium levels (hyperkalemia).

Avoid penicillin and related antibiotics (e.g., cephalosporins). Alert the provider, and monitor for cross-reactivity.
Penicillin can disrupt normal gut flora, potentially leading to diarrhea or superinfections like C. difficile.
Look for signs like rash, itching, hives, or more severe symptoms like swelling and difficulty breathing (anaphylaxis).

Some patients can, but those with a severe penicillin allergy (e.g., anaphylaxis) should generally avoid cephalosporins due to cross-sensitivity.
Alcohol can cause a disulfiram-like reaction with some cephalosporins (e.g., cefotetan), leading to flushing, nausea, and vomiting.
Gastrointestinal upset (nausea, diarrhea), allergic reactions, and potential superinfections (e.g., thrush or yeast infections).

Dairy products and antacids contain calcium and magnesium, which bind to tetracycline and reduce its absorption, making it less effective.
Tetracycline can cause permanent tooth discoloration and affect bone growth in children under 8 years old and in fetuses if taken during pregnancy.
Photosensitivity (increased sunburn risk), gastrointestinal upset (nausea, diarrhea), and potential superinfections like oral thrush or yeast infections.

Absorption is better on an empty stomach, but they can be taken with food if GI upset occurs.
GI upset (nausea, diarrhea, abdominal pain) is common. Rarely, they may cause hepatotoxicity or QT prolongation.
Macrolides inhibit liver enzymes (CYP450), which can increase levels of medications like warfarin or digoxin, leading to potential toxicity.

Calcium and magnesium bind to the drug and reduce its absorption, making it less effective.
Tendon rupture, photosensitivity, and QT prolongation are serious risks to monitor.
They can damage growing cartilage, leading to joint problems.

To prevent crystalluria and kidney stones caused by sulfonamide metabolites.
Allergic reactions, photosensitivity, blood dyscrasias, and Stevens-Johnson syndrome.
They can cause kernicterus (bilirubin-induced brain damage) in neonates.

To ensure the drug is effective without reaching toxic levels that could harm kidneys or hearing.
Nephrotoxicity (kidney damage) and ototoxicity (hearing loss or balance issues).
They are poorly absorbed in the gastrointestinal tract and are more effective when given IV or IM.
Special Offer: 50% Off Nursing 2-Year Survival Package
✅ Make meds finally click
✅ Pass the NCLEX with confidence
✅ Study faster, retain longer, stress less