How to Remember the Causes of Pancreatitis Easily
You can remember the causes of acute pancreatitis using the I GET SMASHED Mnemonic.
Want to learn more?
View a suggested lesson
01.04 Pancreatitis
I GET SMASHED Mnemonic
When I am in the hospital treating pancreatitis, it helps to remember the causes of pancreatitis by using the I GET SMASHED mnemonic. This way, I attend to my patients with ease and prescribe measures accordingly.

The I GET SMASHED mnemonic stands for:
I – idiopathic
G – gallstones
E – EtOH
T – trauma
S – steroids
M – mumps/malignancy
A – autoimmune
S – scorpion stings
H – hypertriglyceridemia/hypercalcemia
E – (post) ERCP
D – drugs (tobacco, thiazides)
View Our Mnemonics Course
210 Lessons
Let’s break down each of the above categories, so you have a better understanding:
Idiopathic
Idiopathic is a term used to describe pancreatitis with no known cause, making the diagnosis of idiopathic pancreatitis difficult. Because of the lack of cause, the treatment also becomes more difficult.
Gallstones
Gallstones are hard deposits typically made of calcium bilirubinate. When gallstones sit in your gallbladder for a long time, they can slowly harden into small stones called “sludge.”
Once the stones are present, they might move up into your common bile duct and block it. The pressure from the blockage can cause infection or pancreatitis.
Ethanol
Alcohol use is one of the leading causes of pancreatitis. When you drink alcohol, the acinar cells in your pancreas metabolize it into toxic substances like free radicals, which can damage the pancreas and cause cell death.
A build-up of these radicals becomes lethal and begins to digest the pancreas itself. The damaged pancreatic tissue causes inflammation which leads to more damage to the pancreas.
Trauma
Trauma has been linked to inflammation and subsequent pancreatitis, such as car crashes or falls injuries. If you hit your vital organ like the pancreas, the cells will die and spill all their content into your bloodstream. For example, a car accident or fall can lead to pancreatitis and gastric irritation from blood loss or stomach acid.
Steroids
The use of long-term steroids has been linked to an increased risk of developing pancreatitis. Corticosteroids treat several conditions, including asthma, congestive heart failure, arthritis, and inflammatory bowel disease. They suppress the immune system, which can trigger pancreatitis.
Mumps
In children, mumps can cause inflammation of the pancreas, which leads to pancreatitis. In adults, this isn’t a common cause of pancreatitis.
It affects adults who have low immunity or never received childhood vaccinations against mumps. When mumps infects your pancreas, it causes the pancreas to become inflamed, which leads to pancreatitis.
Autoimmune
In autoimmune pancreatitis, your body’s immune system mistakenly attacks and damages the pancreas. This can cause inflammation of the pancreas and lead to chronic pain, diabetes, and weight loss.
A heterogeneous autoimmune inflammatory process characterizes autoimmune. This is when prominent lymphocytic infiltration associated with fibrosis of the pancreas causes organ dysfunction. Its cause is still unknown.
Scorpion Sting
There is a rare but deadly risk of pancreatitis from scorpion stings. When a scorpion attacks you, it releases a venom that can irritate the pancreas.
The venom in the sting can cause inflammation and swelling in your pancreas, which leads to pancreatitis.
Hypertriglyceridemia/Hypercalcemia
Both hypertriglyceridemia and hypercalcemia are high levels of certain substances in your blood. Hypertriglyceridemia is high triglycerides, which are a type of fat found in your blood.
High triglycerides can increase the risk of pancreatitis.
Hypercalcemia is high calcium levels in your blood. This can trigger pancreatitis in people who are susceptible to it.
Post ERCP
Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure where doctors use X-rays and a small, flexible tube with a light on the end to look at your digestive system.
ERCP has been known to cause acute pancreatitis. This happens when a bile duct stent is placed mistakenly into the pancreas. Afterward, pancreatitis can develop because of irritation from the procedure.
Drugs
Using several drugs (like tetracyclines, furosemide, azathioprine, tobacco, thiazides for high blood pressure, and beta-blockers) can lead to pancreatitis. The risk of developing pancreatitis with any drug is low; however, the risk becomes greater when multiple drugs are used at once.
Pancreatitis
Pancreatitis is an inflammatory disease of the pancreas. When the pancreas is inflamed, digestive enzymes produced by the pancreas to aid in the digestion of food will begin to digest the pancreas itself.
This can cause pain and damage to the pancreas, mainly if not treated quickly. The inflamed pancreas can also cause the release of toxins and inflammatory cells that can harm your kidneys, lungs, and heart.
Pancreatitis is generally classified as acute or chronic. Acute pancreatitis typically develops very suddenly over a few hours and can sometimes be life-threatening. Chronic pancreatitis is similar to acute pancreatitis in some ways, but it also has long-term consequences due to ongoing damage to the pancreas.
Mild cases of pancreatitis can be treated at home, with rest and a diet that includes easy-to-digest foods. For more severe cases of pancreatitis . . . you will likely need to stay in the hospital for treatment.
Treatment can include IV fluids or a feeding tube to keep you hydrated, pain medication, and antibiotics. The goal of treatment is to resolve the inflammation and allow the pancreas time to heal–which can take weeks or months. If left untreated, pancreatitis can lead to life-threatening complications like organ failure and sepsis.
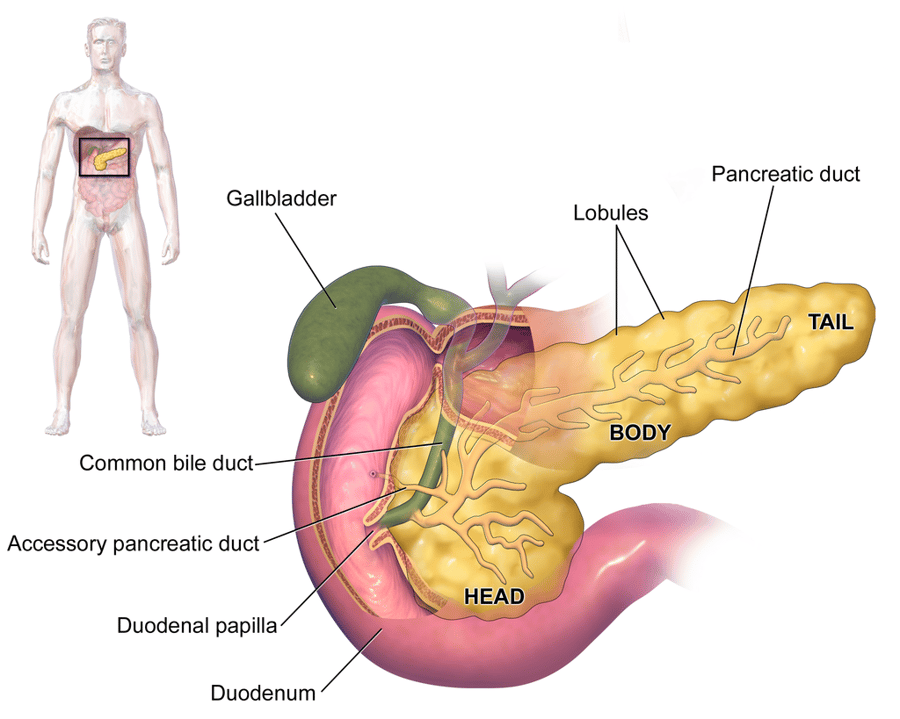
Where is the Pancreas Located, and What Is Its Function?
The pancreas is a glandular organ located in the upper abdomen and connects to the duodenum (beginning of the small intestine). It has a pancreatic duct that drains digestive enzymes into the duodenum.
Your pancreas has two main functions;
- To secrete digestive enzymes
- To release the enzymes into the small intestines
These enzymes help digest food by breaking down carbohydrates, proteins, and fat from food. The pancreas also produces hormones like INSULIN that regulate your blood sugar levels.
What Causes Pancreatitis?
When the pancreas secretes the digestive enzymes, typically, they are inactive until they reach the small intestines. However, when the pancreas is inflamed, the secreted enzymes attack it and damage the tissues that secrete them.
Alcohol and gall stones are the top causes of pancreatitis. As mentioned above, pancreatitis can be either acute or chronic and can lead to complications. In severe cases, bleeding, infection, and permanent tissue damage might occur.
Chronic pancreatitis results from repeated bouts of acute pancreatitis. This causes inflammation and damage to the pancreas, which impairs its ability to secrete enzymes. A poorly functioning pancreas can cause diabetes and digestion complications.
Signs and Symptoms of Pancreatitis
The signs and symptoms of pancreatitis vary, depending on the type of condition:
Acute Pancreatitis Symptoms
If you suffer from acute pancreatitis, you may experience:
- Sudden pain that comes and goes or that builds up over several days
- Moderate or severe belly pain that can spread to your back
- Pain that intensifies when eating
- Swollen, tender abdomen
- Nausea and vomiting
- Fever
- Faster than usual heart rate
Chronic Pancreatitis Symptoms
Chronic pancreatitis may cause similar symptoms as acute pancreatitis. You may also experience:
- Constant, disabling pain that advances to your back
- Unexplained weight loss
- Steatorrhea – foamy diarrhea with visible oil droplets
- Diabetes (high blood sugar) which results when insulin-producing pancreas cells are damaged
This Nursing Mnemonics Course outlines several mnemonics to help you easily remember complex nursing terms. When a patient suffers a sudden pancreatitis attack, the first thing to do is check their level of responsiveness.
Risk Factors of Pancreatitis
Factors that increase your risk of pancreatitis include:
Excessive Alcohol Consumption
Alcohol has been identified as one of the most common causes of pancreatitis. Alcohol can damage your pancreas, making it less able to protect itself from inflammation.
Heavy Smoking
Cigarette smoking or passive smoking is linked to an increased risk of developing acute pancreatitis. Smokers are on average 3X likely to suffer chronic pancreatitis than non-smokers, and current smokers are more likely to suffer acute pancreatitis.
Smoking damages the small blood vessels in your pancreas, which reduces the organ’s ability to heal itself. Quitting smoking decreases the risk of pancreatitis by half.
Obesity
Being overweight or obese is associated with an increased risk of pancreatitis. Carrying excess weight around your mid-section puts pressure on your abdomen, which can cause inflammation that leads to pancreatitis.
Diabetes
Having diabetes increases your risk of pancreatitis. Diabetes damages the pancreas and can cause it to release digestive enzymes that destroy healthy tissue, which leads to inflammation.
Genetics
Having a genetic tendency toward pancreatitis increases your risk of developing the disease. For example, studies have shown that people with the hereditary type of chronic pancreatitis are at an increased risk for acute attacks. If you have a family member who suffers from pancreatitis . . . odds are you may be susceptible to it too.
Complications Resulting from Pancreatitis
Although pancreatitis can be managed and treated with drugs when detected early, it can lead to severe complications when left untreated. They include:
Kidney Failure
A rare complication of pancreatitis is acute renal failure. This happens when the toxins released from the pancreas affect your kidneys, causing them to shut down completely.
If caught early enough, this can be treated with fluids and drugs to help prevent further damage to the kidneys. However, in severe cases . . . dialysis or a kidney transplant may be necessary.
Diabetes
One role of the pancreas is to produce insulin which regulates your blood sugar levels. Damage to insulin-producing cells can cause diabetes. This is because the pancreas is unable to produce enough insulin. This causes your blood sugar level to rise.
Pancreatic Cancer
People with chronic pancreatitis are at an increased risk of developing pancreatic cancer.
Pancreatic cancer is difficult to detect early because there are few noticeable symptoms. This makes it especially dangerous . . . which is why it’s so vital to have pancreatitis regularly monitored.
Are You Struggling With Nursing School? nursing.com/ is Your Savior
I get it. Nursing school isn’t a walk in the park. With numerous study materials, complex units, and the most challenging exams, it can be hard to pass. But that doesn’t have to be the case. At nursing.com/, we offer a multimodal LMS with all learning styles to help students master complex nursing content.
Sign up today and get access to your new online learning system. You’ll interact with videos, simulations, practice tests, live sessions, and tons of other resources designed to help you pass. Seriously. nursing.com/ is . . . a nursing school re-designed.





